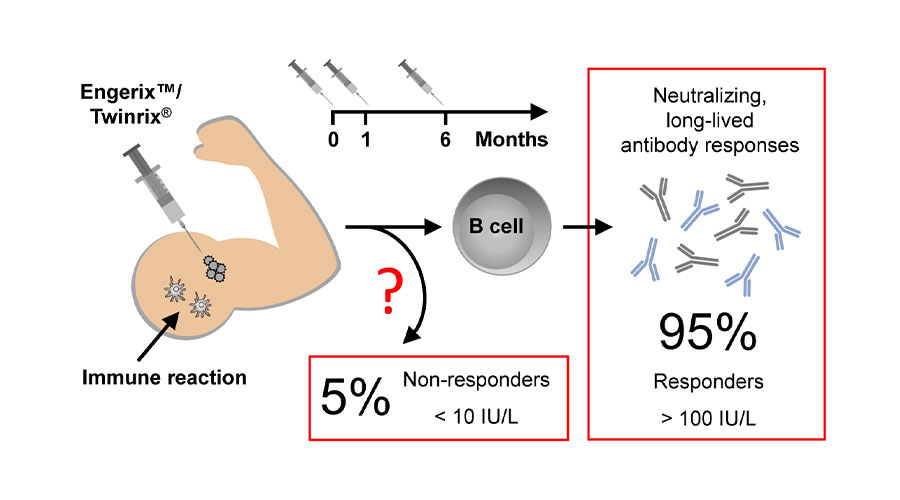
What causes vaccination failure and which new therapies are possible?
What is this research project about?
A vaccination is the best protection against hepatitis B. © Deutsche Leberstiftung
What is this research project about?
Hepatitis B Virus (HBV) infection often causes chronic infection, which may lead to liver cirrhosis that can progress to hepatocellular carcinoma. HBV vaccines are considered highly efficacious and are successfully applied worldwide. However, approximately 5% of HBV vaccinated individuals do not mount protective antibody responses after vaccination (non-responders). Previous studies revealed reduced responsiveness to influenza virus vaccination in the elderly. In contrast, HBV vaccination non-responsiveness cannot be explained by increasing age as also young adults are affected. Consequently, factors causing non-responsiveness are largely unclear.
What’s the current status?
It has been observed that non-responders mostly show an overall normal immunoexcitability and normal responses against many other vaccines. So far, only few molecular parameters have been identified that may play a role in conferring the non-responder status. Different genetic components of the innate and adaptive immune system were discussed to be associated with the phenomenon. Multiple Genome Wide Association Studies (GWAS) claimed that certain genetic factors predispose individuals to HBV vaccination failure. The conclusions of the previous studies range from antigen presentation defects to absence of certain antigen-specific T cells. However, a comprehensive model explaining the phenomenon of HBV vaccination non-responsiveness and biomarkers that allow identification of potential non-responders has not been formulated. Accordingly, no vaccination regimen has been developed that would allow successful vaccination of non-responders. This creates challenges particularly for health care workers who are in frequent contact with patients and therefore are recommended to be vaccinated against HBV. Additionally, it is not clear whether those relatively few individuals who develop chronic infection after HBV exposure during adulthood are also HBV vaccination non-responders.
Even though virus propagation can be inhibited by antiviral therapy, HBV infection cannot be eliminated from chronically infected patients.
How do we get there?
Together with the Occupational Health Physicians of the MHH, we are building up cohorts of HBV vaccination responders and non-responders, which constitute an essential element for research towards the molecular basis of HBV non-responsiveness. Currently, first immunomonitoring studies in HBV vaccinated responders and non-responders are being carried out. Additionally, whole genome sequencing and HLA-typing is being performed to identify genetic characteristics associated with non-responsiveness.

Company doctors at the MHH are working on this RESISIST project.